Senator Edward M. Kennedy’s landmark speech at the 1978 Democratic National Convention in Memphis, Tennessee emphatically brought attention to our nation’s health care dilemma, establishing his stance on health care as a matter of right and not of privilege. The human right to health care means that “services must be accessible, available, acceptable, and of good quality for everyone, on an equitable basis, where and when needed.” Supported by approaches and behavioral science theories, including the Health Belief Model and the Theory of Planned Behavior, mHealth and telemedicine embody the ideals of the right to appropriate care at a suitable time in the correct place.
Decreased Time and Cost of Health Care +
Increased Health of Population and Quality of Care =
High Return on Investments in mHealth and Telemedicine
By incorporating the following five approaches of mHealth and telemedicine into our health care system, lower cost and higher quality care for all becomes a clear reality.
- Remote analysis services. Highly trained professionals work as a pooled resource with fractional employment providing 24/7 coverage with services such as telepathology and teleradiology.
- Remote monitoring technologies. Patients switch from serviced on an inpatient basis to monitored on an ambulatory system.
- mHealth monitoring technologies. Disease managers prevent hospitalization for conditions such as heart failure by accessing daily weight information and proactively assisting patients with fluid retention before a crisis occurs.
- At-home triage services. Televisits from nurses and PCPs decrease emergency room visits.
- Telemedicine appointments. Providers accept patients upon their current availability and
reduce the amount of wasted underutilization.
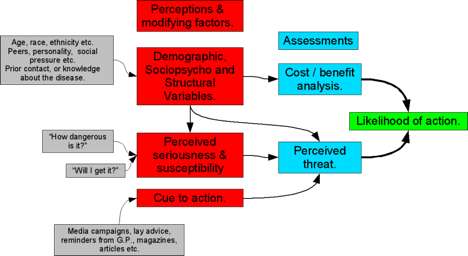
Applying the Health Belief Model to mHealth
 Benefits
Benefits
In a study comparing traditional to mobile app self-monitoring of physical activity (PA), the Health Belief Model (HBM) concept of perceived benefit showed that app users self-monitored exercise more often than non-app users (2.5 days vs 1.25 days per week) and reported greater intentional PA than non app users (150 kcal vs 50 kcal per day).
Barriers
The concept of perceived barrier to wearables involves difficulty with location tracking using Bluetooth (narrowband) and measurable issues in accuracy, time latency, and consistency. Signal strength is an unreliable indicator of distance considering wireless network effects such as obstructions, reflections, refractions, multipath and reception. One innovative solution is ultra wideband (UWB) radio which enables resilient location and distance measurements.
Efficiency of Narrowband vs Ultra Wideband
with Time Latency and Visual Effects
Cues to Action
The concept of cues to action comes to the forefront through instant feedback from such wearables as pedometers or activity monitors. The data acts as a reward when results are high and as a challenging motivator when results are low. Forty percent of trackers indicate that feedback prompts them to ask a doctor new questions or seek a second opinion. Trackers share their results with others in common language in online support groups either to receive and give encouragement or take part in competitions.
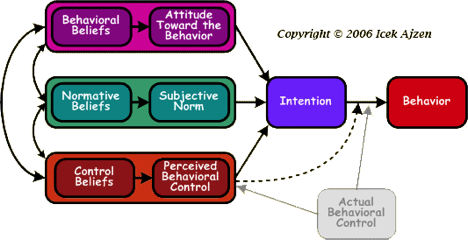
Applying the Theory of Planned Behavior (TPB) to Telemedicine
Subjective Norm
In a study to determine patient use of walk-in clinic telemedicine services for minor ailments compared to emergency room visits, 73% of respondents mentioned that the opinions of their family members would be important considerations. Normative interpersonal channels more strongly influence their decision making than mass media channels which solely gather information.
Perceived Behavioral Control
Perceived e-consultation diagnosticity occurs when the patient believes that images and sounds transmitted through technology are under their control. As remote patients, they perceive that enough accurate information is relayed electronically to allow physicians to understand and evaluate their symptoms and health conditions without being present to “touch and feel” them.
 Attitudes
Attitudes
The attitude of the patient surfaces with increasingly knowing their rights to quality care and believing that telemedicine improves access to quality care. Patients suffering from chronic illnesses that live in rural areas and have limited access to doctors due to disability or age have virtual visits with PCPs or specialists not always available to them.
In conclusion, most Americans are not “at the tip of the iceberg way up high in the health care services” as Senator Kennedy stated in his 1978 convention speech. The road to managing our health care crisis is paved with a golden opportunity. The HBM and TPB behavioral models show that quality care offered universally and equitably at a lower cost is a reality with the growing use of mHealth and telemedicine. Now is the time to allow digital health to propel our nation’s health care system forward to realize our desired outcome.
References:
Darmon, Luc. “Wireless for Wearables.” Embedded Computing Design. (2014)
Newell, Derek. “5 Ways Mobile Apps Will Transform Healthcare.” Forbes. (2012)
Paddock, Catharine, Ph.D. “How Self-Monitoring Is Transforming Health.” Medicine News Today (2013)
Serrano, C. I. and Karahanna, E. “An Exploratory Study of Patient Acceptance of Walk-In Telemedicine Services for Minor Conditions.” International Journal of Healthcare Information Systems and Informatics (IJHISI), 4(4), 37-56. (2009)
Turner-McGrievy G.M., Beets M.W., Moore J.B., Kaczynski A.T., Barr-Anderson D.J. and Tate D.F. “Comparison of Traditional Versus Mobile App Self-Monitoring of Physical Activity and Dietary Intake among Overweight Adults Participating in an mHealth Weight Loss Program.” Journal of American Medical Informatics Association, 20(3), 513–8. (2013)
West, Darrell. “How Mobile Devices are Transforming Healthcare.” Issues in Technology Innovation. Center for Technology Innovation at Brookings. (2012)




 The experience of encountering advertising tailored to one’s behaviors or interests on the internet has become ubiquitous in a very short time. We’ve all had that experience – shopping for a particular shoe on Zappos or gadget on Amazon, not buying it, then having an ad for that shoe or that gadget magically appear in a whole variety of other websites during the course of our browsing over a period of days or even weeks. Or, perhaps, buying that shoe or gadget, and then encountering ads for similar shoes or gadgets, or shoe/gadget accessories.
The experience of encountering advertising tailored to one’s behaviors or interests on the internet has become ubiquitous in a very short time. We’ve all had that experience – shopping for a particular shoe on Zappos or gadget on Amazon, not buying it, then having an ad for that shoe or that gadget magically appear in a whole variety of other websites during the course of our browsing over a period of days or even weeks. Or, perhaps, buying that shoe or gadget, and then encountering ads for similar shoes or gadgets, or shoe/gadget accessories. As Executive Vice President, Angela Tenuta leads client services for
As Executive Vice President, Angela Tenuta leads client services for  Shannon Gallagher serves as Vice President, Analytics Services at Crossix Solutions, where she leads the ongoing expansion of Crossix services and capabilities at the intersection of pharmaceutical and consumer healthcare. A veteran consultant in market research and data analytics for the pharmaceutical, healthcare and CPG sectors, Shannon is passionate about Crossix’s unique position to harness Big Data to empower better communication to the patient as a consumer. Prior to joining Crossix, Shannon spent 10 years working at Nielsen in Innovation Analytics, consulting on new product development for Rx and OTC/CPG manufacturers. Connect with her on
Shannon Gallagher serves as Vice President, Analytics Services at Crossix Solutions, where she leads the ongoing expansion of Crossix services and capabilities at the intersection of pharmaceutical and consumer healthcare. A veteran consultant in market research and data analytics for the pharmaceutical, healthcare and CPG sectors, Shannon is passionate about Crossix’s unique position to harness Big Data to empower better communication to the patient as a consumer. Prior to joining Crossix, Shannon spent 10 years working at Nielsen in Innovation Analytics, consulting on new product development for Rx and OTC/CPG manufacturers. Connect with her on